Many people living with chronic pain are told their MRI is “normal” or that their pain is simply due to wear and tear. But for many patients, the true driver of persistent pain may be something deeper: immune dysfunction and chronic inflammation.
At Barr Center for Innovative Pain & Regenerative Therapies in Virginia Beach, we frequently help patients uncover autoimmune and inflammatory contributors to chronic pain that have gone unrecognized for years.
By identifying and addressing immune dysregulation, we can often improve pain, reduce inflammation, and help patients heal more effectively.
What Is Autoimmunity?
Autoimmunity occurs when the immune system mistakenly attacks the body’s own tissues.
Rather than simply fighting infection, the immune system becomes overactive and creates ongoing inflammation that can damage:
- Joints
- Muscles
- Tendons and ligaments
- Nerves
- Connective tissues
- Internal organs
This chronic inflammatory response can create persistent pain even when structural imaging looks relatively normal.
How Autoimmune Disease Causes Chronic Pain
Autoimmune and inflammatory disorders can directly and indirectly drive pain through several mechanisms:
1. Tissue Inflammation and Damage
Immune attack on joints, connective tissue, or nerves creates inflammation and pain.
2. Nervous System Sensitization
Inflammation can make the nervous system hypersensitive, amplifying pain signals.
3. Poor Healing Capacity
Ongoing immune activation impairs tissue repair and recovery.
4. Central Pain Amplification
Immune activation in the brain and spinal cord can increase pain processing.
Autoimmune Conditions Commonly Associated With Chronic Pain
Many autoimmune and inflammatory disorders can contribute to persistent pain, including:
- Rheumatoid arthritis
- Psoriatic arthritis
- Lupus
- Hashimoto’s thyroiditis
- Sjogren’s syndrome
- Inflammatory bowel disease
- Small fiber neuropathy
- Fibromyalgia-like inflammatory syndromes
- Undifferentiated connective tissue disease
The Role of Neuroinflammation in Chronic Pain
One of the most important emerging concepts in pain medicine is the role of neuroinflammation.
Immune cells in the central nervous system called microglia can become activated by chronic inflammation, infection, trauma, or autoimmune dysfunction.
When activated, microglia release inflammatory chemicals that amplify pain signaling and contribute to:
- Widespread pain
- Nerve pain
- Brain fog
- Fatigue
- Sleep disruption
- Increased pain sensitivity
This is one reason pain may persist even after an injury has structurally healed.
Advanced Therapies That May Help Reduce Autoimmune-Related Pain
At Barr Center, we use a comprehensive functional and regenerative medicine approach to address immune-mediated pain.
Low-Dose Naltrexone (LDN)
LDN may help:
- Modulate immune function
- Calm inflammatory microglia
- Reduce neuroinflammation
- Improve pain sensitivity
- Increase endorphin production
LDN is commonly used in patients with fibromyalgia, autoimmune disease, neuropathic pain, and chronic fatigue.
Peptide Therapy
Certain peptides may support immune modulation and healing.
BPC-157 / TB-500
These may help:
- Reduce inflammation
- Support tendon and ligament healing
- Improve tissue recovery
- Promote nerve repair
KPV Peptide
May help:
- Regulate inflammatory cytokines
- Support gut barrier health
- Reduce systemic immune activation
- Improve autoimmune and inflammatory symptoms
Why a Functional Medicine Approach Matters
Traditional pain treatment often focuses only on symptoms.
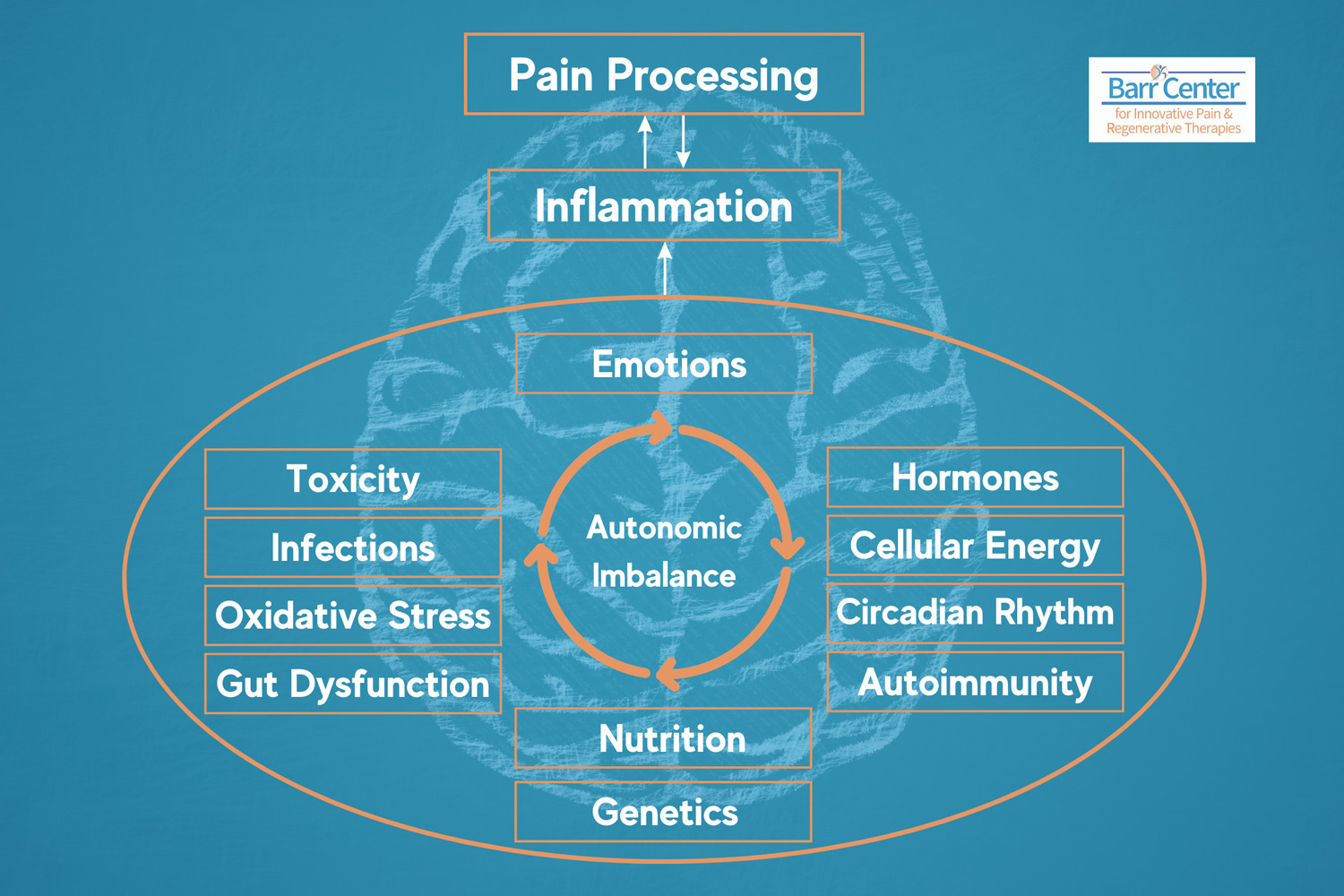
At Barr Center, we look deeper to evaluate for root contributors such as:
- Autoimmunity
- Chronic inflammation
- Gut dysfunction
- Metabolic dysfunction
- Hormonal imbalance
- Nutrient deficiencies
- Neuroinflammation
- Impaired mitochondrial function
Treating the underlying drivers of inflammation can often significantly improve pain outcomes.
Who Should Consider an Autoimmune or Inflammatory Evaluation?
You may benefit from further immune and inflammatory workup if you have:
- Chronic widespread pain
- Pain without clear imaging findings
- Fibromyalgia diagnosis
- Unexplained fatigue with pain
- Brain fog and inflammation
- Slow healing after injury
- Known autoimmune disease
- Persistent tendon or ligament pain
- Neuropathic symptoms
Chronic Pain and Autoimmune Treatment in Virginia Beach
At Barr Center for Innovative Pain & Regenerative Therapies, we specialize in identifying hidden inflammatory and autoimmune contributors to chronic pain.
We serve patients throughout:
- Virginia Beach
- Norfolk
- Chesapeake
- Suffolk
- Hampton Roads
- Outer Banks and Northern North Carolina
Our goal is to help patients reduce pain, restore function, and optimize healing through advanced functional, regenerative, and interventional therapies.
Schedule a Consultation
If chronic pain has not improved despite conventional treatment, immune dysfunction or inflammation may be playing a role.
Contact Barr Center for Innovative Pain & Regenerative Therapies today to schedule an evaluation and learn whether autoimmune or inflammatory factors may be contributing to your pain.
FAQ
Can autoimmune disease cause chronic pain?
Yes. Autoimmune disease can cause inflammation that damages joints, muscles, nerves, and connective tissue, leading to chronic pain.
What is neuroinflammation?
Neuroinflammation refers to inflammation in the brain and spinal cord that can amplify pain signaling and contribute to chronic pain syndromes.
Can low-dose naltrexone help autoimmune pain?
Low-dose naltrexone may help regulate immune activity and reduce neuroinflammation in some chronic pain and autoimmune conditions.
How do you test for autoimmune causes of pain?
Evaluation may include history, physical exam, inflammatory markers, autoimmune labs, metabolic assessment, and functional medicine testing when appropriate.