Glucagon-like peptide-1, or GLP-1, medications are widely known for supporting blood sugar control and weight loss. Emerging research and clinical experience suggest that GLP-1 receptor activation may also help reduce systemic inflammation, improve mitochondrial function, and modulate pain signaling.
At Barr Center and our partner practice, Hang 10, we take a precision-guided, root-cause approach. In select patients, carefully supervised microdosing of GLP-1 medications may help reduce chronic pain and inflammatory burden, often at doses significantly lower than those used for diabetes or weight loss. We have several GLP-1 options available for our patients.
What Are GLP-1 Medications?
GLP-1s are naturally occurring hormones that help regulate blood sugar, reduce insulin resistance, slow gastric emptying, signal satiety in the brain, and reduce inflammatory signaling.
Common GLP-1 receptor agonists include semaglutide, tirzepatide, and liraglutide. While these medications are FDA approved for diabetes and weight management, research suggests they may also have broader anti-inflammatory and neuroprotective effects.
What Is Microdosing?
Microdosing refers to the use of lower-than-standard doses of GLP-1 medications to achieve metabolic and anti-inflammatory benefits while minimizing side effects.
Instead of focusing only on weight loss, microdosing protocols may aim to improve insulin sensitivity, reduce systemic inflammation, lower neuroinflammatory signaling, support mitochondrial efficiency, and reduce central pain sensitization.
Through the careful supervision of the medical staff at Hang 10, patients are monitored for weight, body composition, symptom patterns, metabolic markers, and inflammatory markers. Dosing is individualized, and patients are guided to maintain adequate protein and water intake as appetite decreases. We also assess factors that may limit successful weight loss and create treatment plans to help patients get back on track.
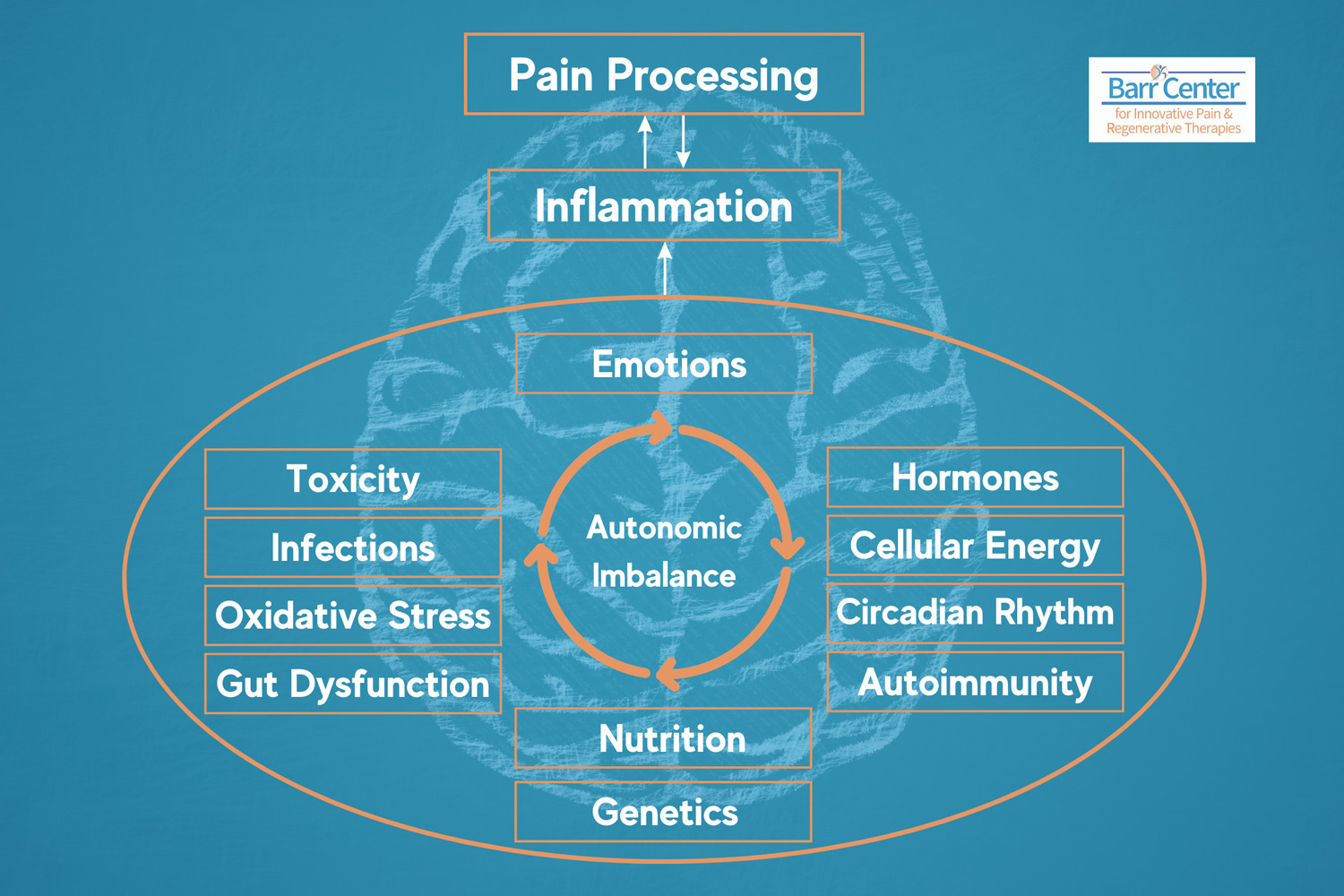
How GLP-1 Activation May Reduce Inflammation
Downregulation of Pro-Inflammatory Cytokines
GLP-1 receptor activation may help reduce inflammatory markers such as TNF-alpha, IL-6, and CRP.
Improved Insulin Sensitivity
Better insulin sensitivity may help reduce oxidative stress and advanced glycation end products that can contribute to inflammation and pain.
Reduced Neuroinflammation
GLP-1 receptors in the brain and spinal cord may help reduce central sensitization and microglial activation.
Mitochondrial Support
GLP-1 signaling may help improve mitochondrial efficiency and cellular energy production.
Conditions That May Benefit
Conditions that may benefit from this approach can include chronic low back pain, osteoarthritis, peripheral neuropathy, fibromyalgia, autoimmune-related pain, post-COVID inflammatory syndromes, and metabolic-associated joint pain.
Potential Benefits
Patients may experience reduced joint pain, improved morning stiffness, better energy, reduced brain fog, improved body composition, and lower inflammatory markers, even without significant weight loss.
Safety Considerations
GLP-1 medications are generally well tolerated when prescribed and monitored appropriately. They may not be appropriate for individuals with a personal or family history of medullary thyroid carcinoma, MEN2 syndrome, severe gastroparesis, or certain pancreatic conditions.
A medical evaluation and baseline labs are recommended before starting treatment, and periodic lab monitoring is also advised.
GLP-1 Microdosing in Virginia Beach
At Barr Center for Innovative Pain & Regenerative Therapies, in conjunction with Hang 10 in Virginia Beach, we evaluate chronic pain through a metabolic and cellular lens. Microdosing GLP-1 therapy represents one of several innovative tools used to help patients reduce inflammation, restore function, and reclaim quality of life.
To learn more, call Hang 10 at 757-974-5828.