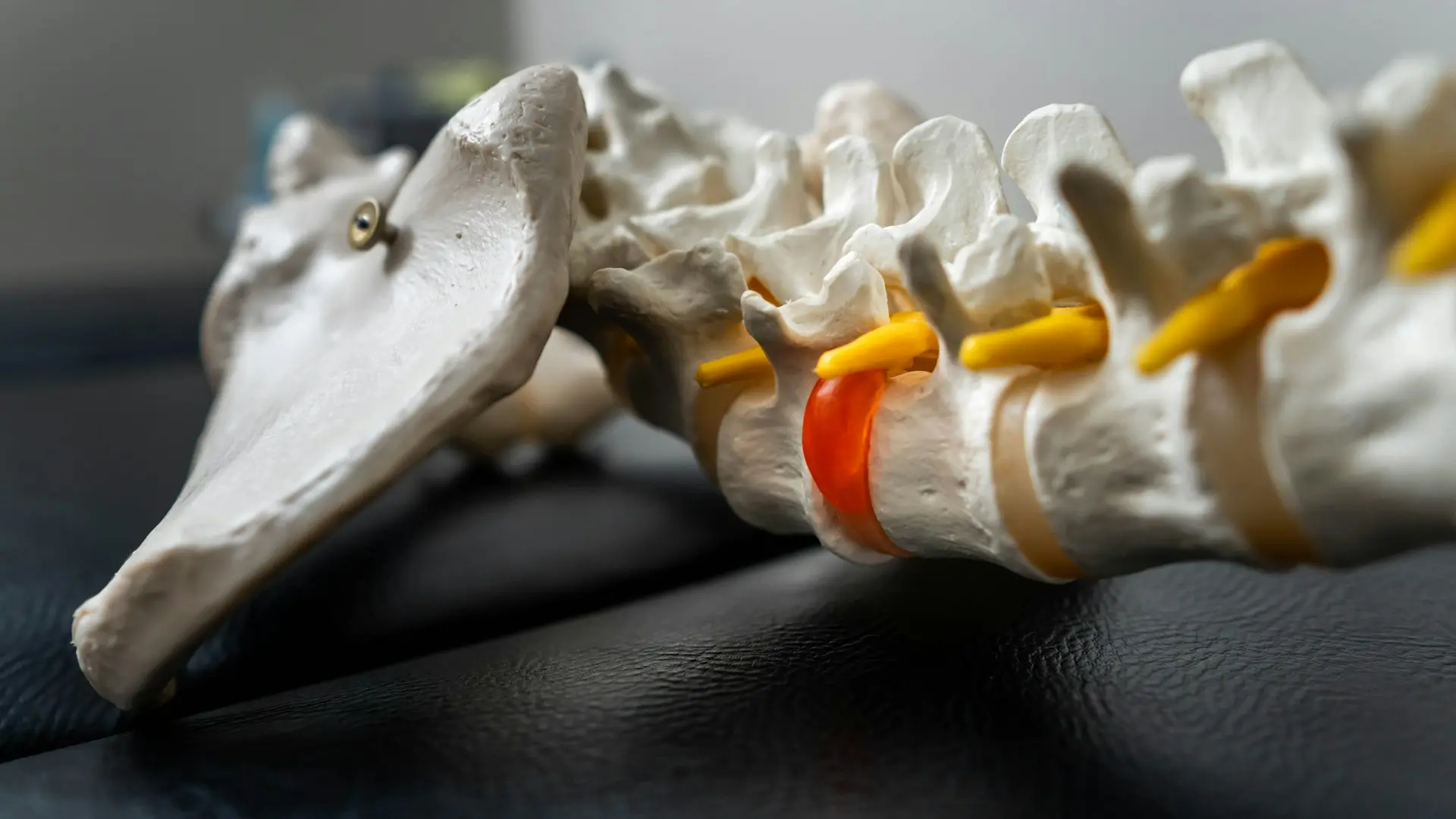
Internal disc disruption is best understood in the lumbar spine, because it is more common in occurrence and the anatomy is easier to understand. It can cause episodes of severe low back pain with muscle spasms. Discogenic pain symptoms are usually exacerbated by sitting for long periods, bending and lifting. In rare instances the symptoms may become constant. We call this discogenic pain. This is in contrast to when a lumbar herniated disc presses against a nerve root causing sciatic pain, numbness, and/or weakness in your leg. Internal disc disruption is sometimes referred to as a leaky disc phenomenon. This means that pain can occur from “leaking” of nuclear disc material through an annular tear as opposed to an actual herniation of the disc. This can lead to irritation of a variety of pain sensitive structures in the spine.
Provocative Discography
It is a diagnostic test to assess if small tears within the disc that can cause discogenic back pain. Contrast dye is injected into the disc nucleus (the gel-like substance in the center of the disc). This is the only diagnostic test that provides both anatomical and functional information about a diseased disc causing discogenic pain, and can identify problems that may not be seen on MRI or CT. Discography is also helpful in specifically localizing the disc level that needs to be treated.
 Who can benefit from discography?
Who can benefit from discography?
Discography is considered an invasive diagnostic test and is performed only when the information is needed for surgical or other intradiscal intervention decision-making. More conservative treatments such as physical therapy and therapeutic spinal injections are typically prescribed before considering provocative discography.
How is the procedure done?
This procedure is done with the patient lying on his or her stomach. Typically, a mild sedative is given through an IV. The patient remains awake but sedated during the procedure. The skin and soft tissues are anesthetized.
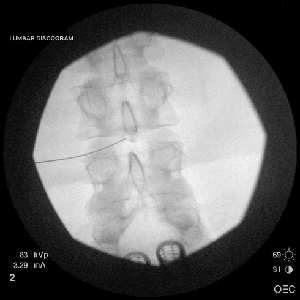
Under fluoroscopic (X-ray) guidance, Dr. Barr will insert a needle into the disc. Contrast dye is injected and an X-ray (discogram) is taken, which may show tears in the outer portion of the disc (annulus).
During the disc injection portion of the procedure, the patient will be asked if the increased pressure in the disc causes discomfort. Specifically, the patient will be asked to describe any discomfort with particular attention to the reproduction of the patient’s “typical back pain” in quality and location. Those disc injections which reproduce the patient’s “typical back pain” and have evidence of tears within the annulus (outer portion of the disc) are considered positive and likely are the etiology of the patient’s back pain.
Pain medication is usually given during and after the procedure. The procedure takes approximately 45-60 minutes.
Is the procedure painful?
Because there is typically some discomfort during the procedure, a mild sedative and pain medication are usually given by IV. Most patients tolerate the procedure quite well. They are usually sore for a few days to two weeks after the procedure, and pain medication may be needed for a few days afterward. Ice may be applied to the region as needed.
What should I do after the procedure?
- Take it easy for the next few days.
- Most patients take off work the next day.
- Your physician will let you know of any activity restrictions.
Are there any contraindications to provocation discography?
Contraindications to discography include the following:
- Patients with a bleeding disorder or on blood thinners
- Pregnancy
- Any systemic infection or local skin infection over the puncture site
Are there any risks to the procedure?
Some discomfort is to be expected, but it should be temporary.
Other side effects of the procedure are extremely rare and include:
- Worsening of symptoms
- Infection
- Bleeding
- Discitis—a serious but extremely rare infection of the disc itself (antibiotics are given via IV or in the disc to help prevent this)
- Nerve or spinal cord injury
Can the Barr Center Help You with Back Pain Relief?
Call us at 757-578-2260 or email us at Info@BarrCenter.com to get started on relieving your back pain.
Learn More
Other pain management conditions we treat are: Neck Pain, Shoulder Pain, Hip Pain and Knee Pain. We often use Regenerative Medicineand Physical Therapy in our treatments.